

People on Medicaid usually need to confirm their eligibility every year in order to renew their coverage. During the COVID-19 pandemic, however, all states paused the annual renewal process and provided continuous healthcare coverage for approximately 3 years. As a result, the number of people on Medicaid swelled to 94 million—the highest level in history.
In May 2023, the COVID-19 Public Health Emergency ended and annual renewals resumed. Based on historical precedent, it was estimated that around 6.8 million people were at risk of losing their healthcare coverage, despite being eligible.
To prevent eligible members from losing their coverage, my team partnered with state Medicaid programs to rapidly improve their renewals processes

Our team of 10 divided up roles for each state we partnered with. Generally for each state we’d have around half the team working as the primary team, including participating in site visits, and the rest of the team offering virtual secondary support. I served as a design lead for 4 state visits and as a support for an additional 4 states
I developed a funnel template which helped our state partners to visualize their data, and understand how the phases of the renewal process were connected and clearly see where the top areas to focus our interventions on. This was a novel approach for most of our state partners, who often approached their data piecemeal rather than holistically.
Example: In one state we could see that nearly half of all members who needed to complete the manual process never submitted their forms, resulting in being denied on procedural grounds.
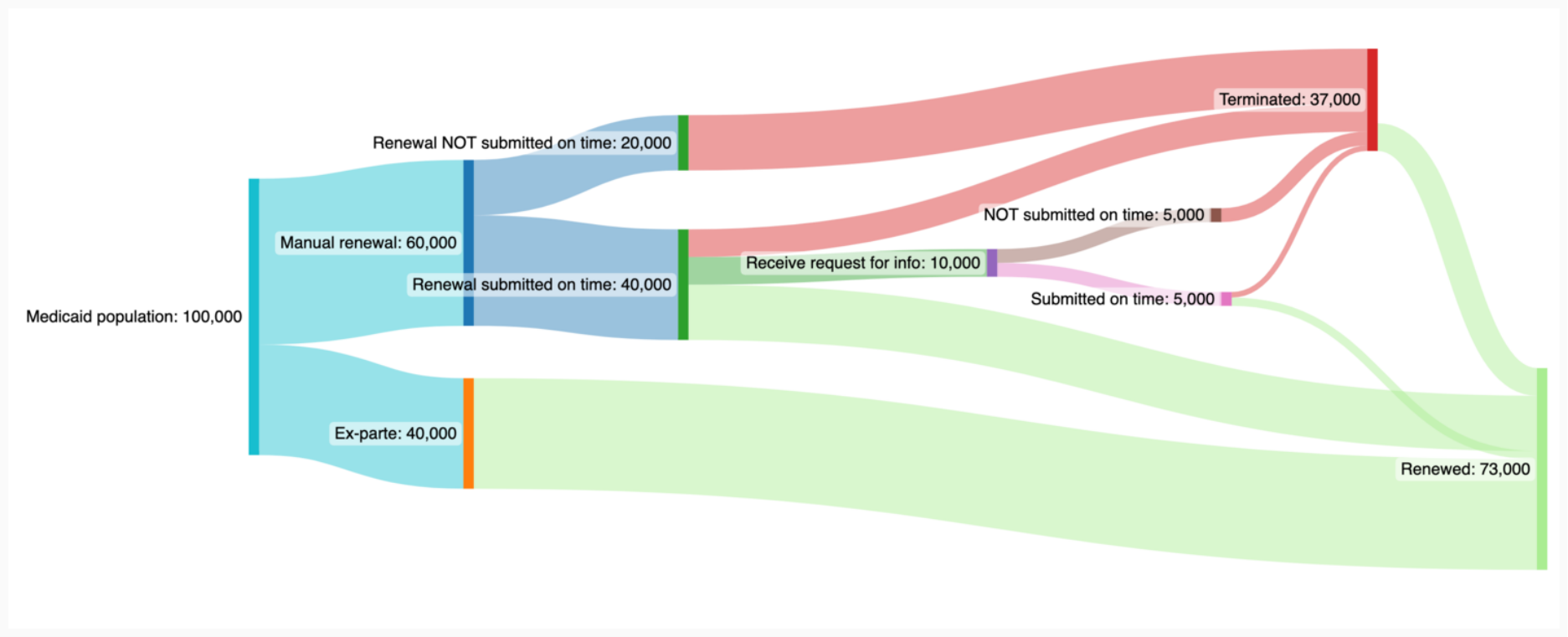
To answered that question, our engineers worked with state staff to pull system data and I did user research with Medicaid members and front-line workers to answer questions such as
Example: Research revealed that one reason members were not completing their renewals is because they mistakenly thought mailed renewal notices were spam, and often threw them away without ever opening them.

We brought together community-based organizations who assist members in navigating the application and renewals process to participate in a workshop to co-design solutions. As front-line workers, they had deep subject matter expertise in the needs of their communities. I opened the workshop by reviewing some of the top challenges we identified through user research, then broke everyone into smaller groups to brainstorm solutions on sticky notes. We then grouped similar stickies and talked through the ideas together.
Example: In one such workshop, participants brought forward the idea to redesign the envelopes to make it more clear that there was actionable content inside

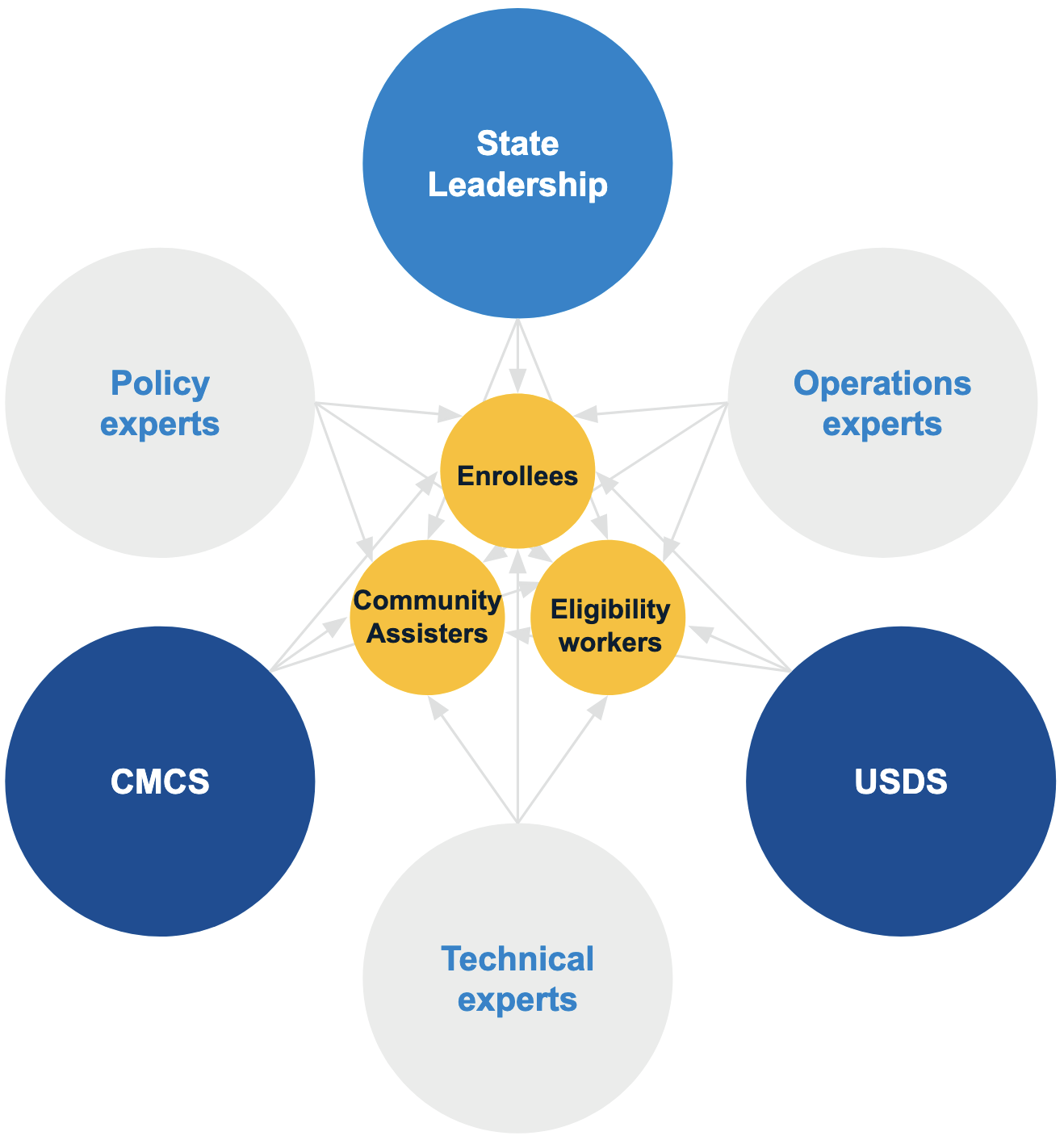
Over the course of a 1-week onsite visit, we convened all stakeholders into one room for the duration of the onsite. This included state leadership, eligibility workers, and implementation staff to review the research done to date and then work together to prioritize and initiate new approaches together. Often, it was the first time these groups had ever been in a room together.
I helped facilitate conversations to bridge the gap between what should be happening, the reality discovered in our research, and what it would take for implementation teams to make changes. With leadership in the room, we were able to capture decision making in real time.
By centering the conversations around the needs and challenges of those experiencing the renewals process directly— enrollees, community assisters, and state eligibility workers—we empowered the states to make rapid adjustments that had a big impact.
At the end of a one week onsite, our team would deliver a list of actionable recommendations based on research findings and solutions developed during onsite workshops. Recommendations were organized based on estimated impact and level of effort
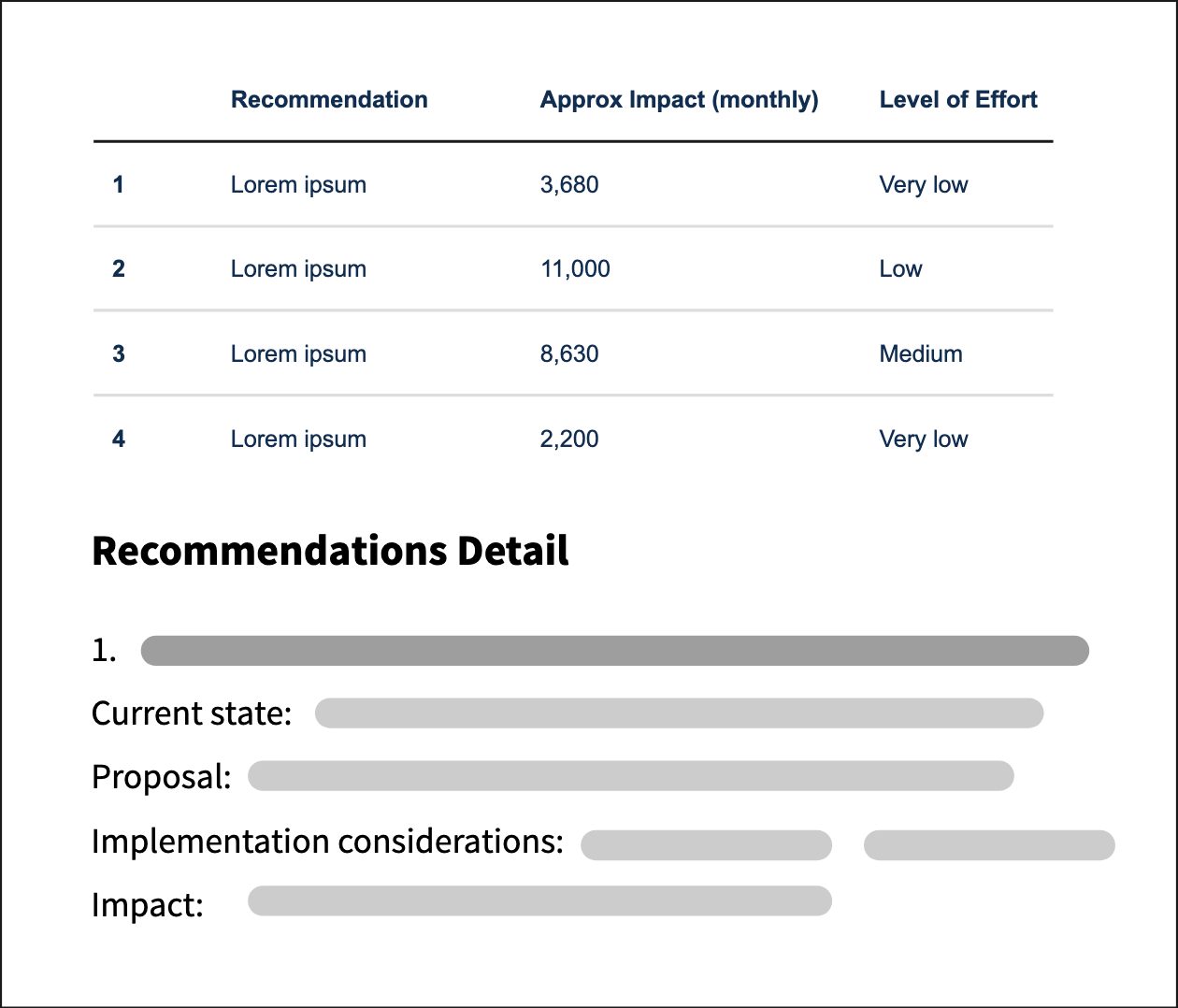
In the 2–3 weeks after each onsite, we worked with states to implement the recommendations. This ranged from pushing vendors to meet timelines to implementing specific changes.
Example: I redesigned the renewal envelope for New York to make it distinct from other mailings with a call to action in 19 languages

additional Americans estimated to be renewed for health coverage via ex parte (automated) processing in 2024
hours of eligibility worker processing time estimated to be saved in 2024
supported through in-depth technical assistance across diverse geographies, populations, and needs
children and families reinstated for coverage across 29 states as a result of actions taken by CMCS and supported by USDS